Reading time: 8 min.
Worried about hair transplant anesthesia? This clear, patient-first guide explains how numbing works, the drugs commonly used, what you’ll feel (and won’t), how clinics keep you safe, and the questions to ask before you book.
Know a friend anxious about pain? Share this guide before they book.
Quick Take
Most modern transplants use local anesthesia (e.g., lidocaine with epinephrine) with or without light sedation; general anesthesia is rarely necessary.
Comfort is maximized with nerve blocks, buffered local, slow injection, vibration/ice, and tumescent solution to prolong numbness.
Ask who administers and monitors anesthesia, what drugs are used, and the plan to treat pain/anxiety before, during, after.
Red flags: no physician present for anesthesia decisions, unclear monitoring, or promises of “no needles” without detailing alternatives.
After effects are usually mild (tenderness, tightness). You’ll receive instructions on icing, sleep position, and medication timing.
Related reading: Hair Transplant Cost Comparison • FUE vs FUT Hair Transplant • Before You Choose a Hair Transplant Surgeon • How to Choose the Best Hair Transplant Clinic
Why Anesthesia Choice Matters In Hair Surgery
A transplant is a long, meticulous procedure. Good anesthesia keeps you comfortable, keeps the field bloodless enough to work precisely, and allows the surgeon to focus on donor protection and natural design. Your anesthesia plan should be tailored to your health, anxiety level, and session length.
Your Options At A Glance
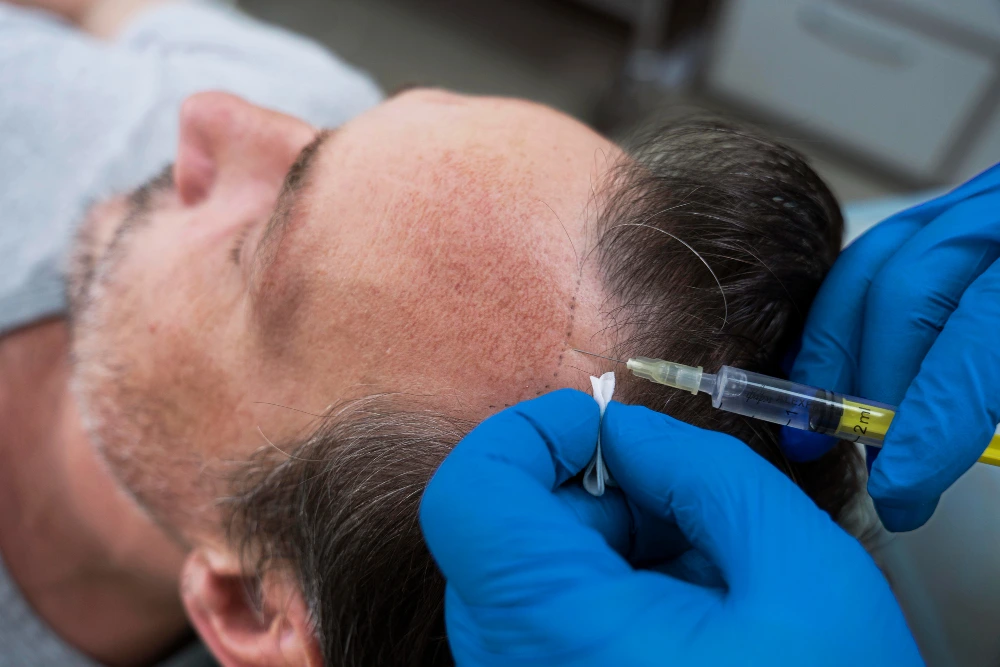
Local anesthesia (standard of care)
- What it is: Injections that numb the scalp in donor and recipient areas.
- Common agents: Lidocaine and/or bupivacaine, often with epinephrine to reduce bleeding and extend effect.
- How it feels: A few minutes of stinging/pressure during initial injections; then numb.
- Why it’s used: Reliable, allows you to stay awake, and avoids the risks of general anesthesia.
Tumescent anesthesia (supportive)
- What it is: Dilute anesthetic/epinephrine solution infiltrated under the scalp.
- Benefits: Prolongs numbness, creates gentle tissue separation for graft placement, and reduces bleeding.
Sedation (optional, case by case)
- Oral anxiolysis: A single tablet (e.g., benzodiazepine) to take the edge off; you must have an escort home.
- IV conscious sedation: Titrated by an appropriately trained professional; you’re responsive but relaxed, with continuous monitoring (pulse oximetry, blood pressure, ECG as indicated).
General anesthesia (rare)
- When considered: Complex combined procedures in a hospital setting or special circumstances.
- Trade-offs: Requires an anesthetist, airway management, and hospital-level monitoring; not typically needed for FUE/FUT alone.
Making Local More Comfortable: Techniques That Help
- Nerve blocks first: Supraorbital, supratrochlear, auriculotemporal, occipital blocks reduce the number of skin sticks.
- Buffered anesthesia: Mixing lidocaine with bicarbonate reduces sting.
- Slow injection + small needles: Dramatically lowers discomfort.
- Vibration/ice distraction: Competes with pain signals; simple and effective.
- Staged numbing: Top-ups during long cases to keep you comfortable.
Safety Checklist (Before You Say “Yes”)
- Medical history review: Allergies, meds (especially blood thinners), prior anesthesia reactions, sleep apnea, heart/liver issues.
- Who’s in charge: A physician determines the anesthesia plan and supervises; support staff work within their licensed scope.
- Monitoring: At minimum pulse oximetry and blood pressure; longer or sedated cases may add ECG/CO₂ monitoring.
- Drug limits: Lidocaine/bupivacaine dosing follows weight-based safety thresholds; clinic should track cumulative totals.
- Emergency kit & training: Oxygen, airways, reversal agents (e.g., benzodiazepine antagonist if used), and a documented escalation pathway.
- Consent: You’re told what drugs are planned, possible side effects, and alternatives.
Red flag: “We don’t really monitor because it’s just local.” Even local needs basic monitoring and documentation.
What You’ll Feel: A Realistic Timeline
- Prep (10–20 min): Photos, marking, vitals.
- Initial numbing (5–10 min): Brief stinging/pressure; usually the most uncomfortable part.
- Harvest phase (FUE/FUT): You should feel pressure, not pain. You can chat, nap, or watch a screen.
- Recipient-site creation & placement: Periodic top-ups keep the area numb.
- Wrap-up: Tenderness or tightness as local wears off; take medications as instructed.
Aftercare For Anesthesia
- Day 0–1: Mild tenderness; use prescribed analgesic (often acetaminophen ± a short NSAID course if allowed).
- Sleep position: Head elevated; small travel pillow helps.
- Icing: Around (not on) recipient sites to reduce forehead swelling.
- Numb spots: Small patches can last days–weeks; usually self-resolve.
- Call the clinic: If you notice spreading numbness, increasing pain, dizziness, or rash.
Special Considerations
- Adrenaline sensitivity: If you’re sensitive to epinephrine (palpitations, tremor), tell your team; they can adjust concentration or technique.
- Lidocaine allergy (rare): True allergy is uncommon; alternatives or preservative-free formulations may be used after physician review.
- Sleep apnea / high BMI: Sedation plans and positioning are modified; you may be asked to bring your CPAP.
- Long sessions: Breaks, hydration, and staged anesthesia maintain comfort and safety.
Questions To Ask Your Surgeon (Copy/Paste)
- Who administers and monitors my anesthesia? Will a physician be present throughout?
- Which local agents and doses do you typically use? Do you buffer injections?
- What monitoring is in place (pulse ox, BP, ECG if sedated)?
- Can I have oral or IV sedation? What are the pros/cons for me?
- How will you keep me comfortable during top-ups in a long session?
- What are the side effects I should expect the first 24–48 hours?
Hair Transplant Anesthesia & Technique
Technique choice influences anesthesia details. FUE often uses broader tumescent infiltration across the donor; FUT numbs a linear strip area and may include additional blocks for closure comfort. In both, the goal is the same: steady analgesia with minimal bleeding, so placement quality stays high.
See Top-Rated Clinics
Prefer a diagnosis-first approach? Browse neutral, vetted clinics that manage genetic hair loss with medical therapy (and surgery if needed). Filter by credentials, outcomes, and follow-up care. → See top-rated clinics
Hair Enhancement Resources & Guides
- Hair Transplant Cost Comparison — how prices vary and what you’re paying for.
- Hair Transplant Cost Calculators & Pricing Factors — use calculators wisely and compare total value.
- How To Choose The Best Hair Transplant Clinic — pre-booking checklist and red flags.
- FUE Vs FUT Hair Transplant — pros/cons and donor strategy (affects cost).
- Hair Transplant Recovery Timeline — plan time off and aftercare costs.
- Patient Photo Standards: How to Read Before/After — verify value with honest results.
- Effective Non-Surgical Hair Restoration Methods — ways to improve yield and reduce repeat spend.
FAQ
Bottom Line
Done properly, hair transplant anesthesia is safe, predictable, and customized to your comfort level. Expect local anesthesia (with or without light sedation), continuous monitoring, and a clear plan for pain control during and after the procedure. Choose clinics where a physician oversees anesthesia decisions—and where your questions are answered in plain English.
Was this helpful? Share our anesthesia guide so others know what to expect and book with confidence.
References
- NHS — Hair transplant (what it involves, anaesthetic & day-case info).
- NHS — Local anaesthesia (uses, risks, side effects).
- American Society of Plastic Surgeons (ASPS) — Hair transplant preparation (anaesthesia types).
- International Society of Hair Restoration Surgery (ISHRS) — Anesthesia in hair restoration (patient education).
- ISHRS Hair Transplant Forum — Buffering local anaesthetic (reducing injection pain).
- ASDSA (Dermatologic Surgery) — Position statement on office-based surgery (sedation & airway competence).
- American Society of Anesthesiologists (ASA) — Standards for basic anesthetic monitoring.
- ASA Practice Guidelines — Moderate procedural sedation/analgesia (2018).
- BHNS (UK) Patient Leaflet — Hair transplantation (local anaesthesia, day-case).
Medical Disclaimer: The content on hairimplants.net is for informational purposes only and should not be considered medical advice. It does not replace a professional medical consultation, diagnosis, or treatment. Readers are encouraged to seek guidance from a qualified healthcare provider before making any decisions about hair restoration treatments. Hairimplants.net accepts no liability for actions taken based on the information provided.
Affiliate Disclosure: Hairimplants.net may contain affiliate links. If you click a link and make a purchase, we may earn a small commission at no additional cost to you. This helps us keep our content free and research-based. Our editorial opinions are independent and not influenced by partnerships. We do not accept payment for favorable reviews or rankings. Links to medical sources are non-affiliate.